“Palliative care aims to improve a person’s quality of life through improved symptom management while addressing psychosocial, emotional and spiritual issues. It is care that is appropriate at all stages of a person’s illness. An interdisciplinary care team may involve medical oncologists, radiation oncologists, family physicians, palliative care physicians, social workers, dietitians, nurses, spiritual care workers and other health professionals” CANCER CARE ONTARIO
Palliative care can be separated into three stages. These stages enable the caregiver to plan and work with expected outcomes. A palliative performance scale tool was developed by Victoria Hospice Society, and is available at Cancer Care Ontario web site. Use of this tool gives the caregiver information to support and anticipate level of care required.
- PPS level — 100% – 70% — Stable stage
- PPS level — 60% – 40% — Transitional stage
- PPS level — 30% – 0% — End of life stage
In each of these stages symptom management is required, the following pages cover the most common symptoms.
Pain
Pain is a common symptom in palliative or end of life care. Pain has several origins.
- Due to the disease itself
- Due to the investigation and treatment of the disease
- A result of a complication of the disease or treatment
- Unrelated to the cancer(2)
The origin of pain is not limited to the physical body, pain may be a combination of emotional and spiritual suffering, this is referred to as “total pain”. To effectively manage pain the whole person must be assessed.
A pain score, greater than 5 on a 0-10 scale requires the use pain medication, in conjunction with relaxation techniques, massage and any other therapeutic techniques that the patient and caregiver find effective. Pain medication combines opoids, anti-inflammatories, and a group of medications referred to as adjuncts in order to maintain a pain score of less than 5. In order to create a safe and effective pain relief cocktail there will be a need to involve a prescriber (Nurse Practitioner or Doctor) and a Registered Nurse to ensure effective outcomes and assess for side effects, intolerance and complications.
Emotional and spiritual pain can be a result of isolation, unresolved family and personal issues, feelings of loss, grief, alterations to independence and other changes that come with the end of life. The caregiver, should encourage communication of painful or positive thoughts and feelings, talk about contributions to life, victories in life, encourage the participation family and friends. If appropriate ask the patient how she/he wants life to end. Grief counselors are also available through palliative support groups. www.cancer.ca has links to support groups.
Spiritual pain is harder to assess as we all have varying spiritual beliefs and concepts. In the developmentally delayed population this concept may be vague therefore difficult to discuss. All humans have a concept of something greater than ourselves, understanding this concept and accepting our powerlessness to change the outcome of the life cycle may complicate pain until acceptance is achieved.
Touching, holding hands, singing and music can initiate a spiritual experience when words cannot, this connection may promote a sense of peace and serenity.
Bowels
Constipation, in palliative care is a condition that requires preventative therapies and maintenance. All cancer or palliative care patients must be on or have access to a bowel routine which includes use of laxatives and stool softeners.
Complications: unresolved constipation will lead to bowel obstruction which will require medical intervention. Constipation can occur even with reduced food intake.
Some signs of bowel obstruction:
- Nausea and vomiting
- Abdominal pain and distention
- Unable to pass gas
Common signs of constipation:
- No bowel movement after 3 days or no movement 1-2 days longer than the individual’s normal routine
- Difficulty passing stools
- Feeling the need to go and only producing watery stools without relief
- Stomach distention, with stomach pain or cramping
- Reduced appetite in conjunction with the above signs
Good bowel management starts with knowing the risks or causes. Examples of risk and causes:
- Reduced fluid intake especially water
- Inappropriate use or poor use of laxatives and stool softeners
- A side effect of medications (especially opoids/pain meds)
- A side effect of some treatments (for example chemotherapy)
- Reduced activity
- Part of the disease process (mechanical bowel obstruction related to a tumour)
Recommendations:
- Daily use of laxatives and stool softeners
- Maintain a bowel chart (frequency, type, difficulty/ease)
- Consult with a community nurse through your GP or CCAC
- Consult with the attending doctor or nurse practitioner
Nausea
Nausea, (and vomiting) can be caused by medications, therapies (chemotherapy/radiation), constipation and bowel obstruction. “The prevalence of chronic nausea in patients with advanced cancer varies from 20%-70%” (Alberta Hospice Palliative Care Resource Manual p.59). An accepted tool to gage the intensity of the nausea is called the Visual Analogue Scale (VAS).
Recommendations:
- observe for nausea trends, when does the nausea occur?
- Avoid spicy, greasy, odorous foods
- Provide calm meal times, and small portions of food
- Use anti-nausea medication as prescribed
- Check for constipation, and provide good oral hygiene
- If nausea does not improve have doctor or CCAC send in a nurse to assess
Appetite
Anorexia is a common symptom in cancer care especially in the palliative stages. There is not usually one identifiable cause, “Cancer anorexia/cachexia occurs in 80%-90% of patients with advanced cancer.” (Alberta Hospice Palliative Care Resource Manual p.55.)
Anorexia is harder on the family/caregiver than the patient. Families feel that if only their loved one will eat he/she will feel better, get stronger, live longer, support is needed to move away from these beliefs and embrace quality of life.
Recommendations:
- Avoid forcing food. This can lead to complications such as aspiration, vomiting, abdominal distention due to poor food digestion and absorption
- Consult with prescriber, there may be a case for an appetite stimulant
- Encourage favorite foods in small frequent amounts
- Use soft, pureed foods or liquid meals for easier swallowing and digesting
- Provide good mouth care and observe mouth for evidence of thrush or ulcerations
Hydration
Hydration in palliative care is not a standard procedure or therapy. Usually there has to be a specific indication such as delirium or opoid toxicity. “Patients who develop delirium or opoid toxicity may benefit from parenteral hydration if the oral route is not feasible.” (Alberta Hospice Palliative Care Resource Manual P.48.) If hydration is ordered the most suitable route for the patient is subcutaneous, also called hypodermoclysis. Hypodermoclysis is the insertion of a tiny needle into the fat of the skin. The benefits of this method include:
- Easier access, veins may be difficult and painful to access
- Less invasive than IV
- Can be given easily and safely at home
- Site can last up to 7 days, IV sites need to be changed every 3 days
- Less risk of systemic overload with saline (Alberta Hospice Palliative Care Resource Manual p.47)
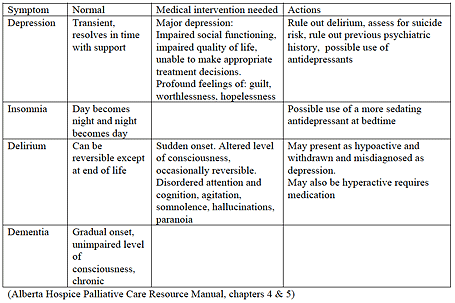
Mood disorders
Mood disorders can include depression, anxiety, confusion, insomnia and some forms of dementia.
Shortness of Breath (Dyspnea) Cough & Fatigue
Shortness of breath (SOB) is a very distressing symptom, combined with cough and fatigue it becomes more difficult to manage and promotes anxiety in the patient and family. Mild SOB can be tolerated and may have minimal effect on the patient’s ability to be involved in day to day activities. When SOB is distressing to the individual, caregivers must engage in managing activities to promote rest and energy conservation. Often the patient’s perception of SOB is different than the observer.
“Dyspnea is an uncomfortable awareness of breathing. Like pain, it is a subjective sensation, involving both the perception of breathlessness and the patient’s reaction to it.” (Alberta Hospice Palliative Care Resource Manual p.51)
If oxygen is prescribed and available then it should be used in conjunction with rest, calm and energy conserving activities. Cough suppressants can be used (as prescribed) to reduce the cough and provide rest intervals between coughing sessions. If the cough is producing blood tinged, yellow or green sputum, there will be a need for a medical assessment as there may be a lung infection that is contributing to the SOB.
“Maintaining high fowler’s position, bed rest, good oral hygiene, and increased ventilation are all easy measures to decrease perception of dyspnea” (Alberta Hospice Palliative Care Resource Manual p.51.)
Increasing fatigue and SOB with activity and a PPS score above 50% may be an indicator of reduced hemoglobin. A PPS score of below 50% in conjunction with increasing fatigue and SOB at rest may indicate impending death. The involvement of a Registered Nurse will provide the support required to communicate with a prescriber to meet the needs appropriately.
References
-
- Cancer Care Ontario, https://www.cancercareontario.ca/en
- Managing Cancer Pain, The Canadian Healthcare Professional’s Reference, Copyright 2005, Perdue Pharma
- Alberta Hospice Palliative Care Resource Manual, 2001
Written by Aakilah Ade RN Certified Hospice and Palliative Care Consultant, 2012 aakilahade@hotmail.com
